On Chronic Pain and Disability
Please click here to read the full FTC Affiliate Disclosure policy.
- December 9, 2025 @ 13:33 pm EST
- comments

If there is an area where medicine really seems to fail patients, it is chronic pain. Most of the world over, if you get trapped in a pain syndrome, your symptoms can be only managed, sometimes only marginally. It is rarely completely cured, and living with pain and disability often becomes your normal. Uncured pain is all too often the pathway to the cliff that is opioid addiction. Furthermore, a frightening analysis showed that overuse of NSAIDs, which are frequently given to manage pain, increases the risk of a cardiovascular incident.
I’m the medical writer for a brilliant physician (full disclosure: she is also my mother) who has made huge strides in treating chronic pain conditions that people largely consider uncurable. She has done this by comprehensively treating the myofascial (muscle) component of pain, in addition to the neuropathic (nerve) component. Her treatments not only relieve pain, but also disability, and her patients become pain-free while tapering off/greatly reducing or entirely weaning off pain medications.
In writing for her, and also being her patient (she treated me for a type of carpal tunnel), I’ve come to realize that the reason pain management is such a mess is this: muscle pathology (manifesting as myofascial pain), while being a huge aspect of pain syndromes, is inadequately addressed by the medical establishment. Muscle pain and disability are not treated by doctors, but referred to physical therapists and chiropractors. Neither group has managed to address it comprehensively – the rest of this post makes a valiant attempt to explain why.
She treats myofascial pain through a well-established technique called dry needling, which, though poorly understood mechanisms, relieves the myofascial trigger point, and also promotes increased blood flow to muscles, promoting healing. As the review I cited discusses, dry needling of deeper muscles is far more effective, but is avoided because it is inherently risky. She has managed to near-eliminate that risk by doing dry needling under ultrasound guidance, to visualize and control the needle path.
Importantly, her ultrasound-guided dry needling technique differs almost entirely from the dry needling done in the US. Using ultrasound, which can detect the local twitch response elicited by a needle that is characteristic of a trigger point, she discovered that myofascial trigger points are numerous, far more so than what is currently fathomed by anyone else in the medical field. There are a multitude of trigger points in superficial, shallow, and deep-seated muscles. To effectively fix myofascial pain, one has to relieve all or most of these trigger points. No one seems to be taking that approach, and consequently, pain remains uncured and disability persists.
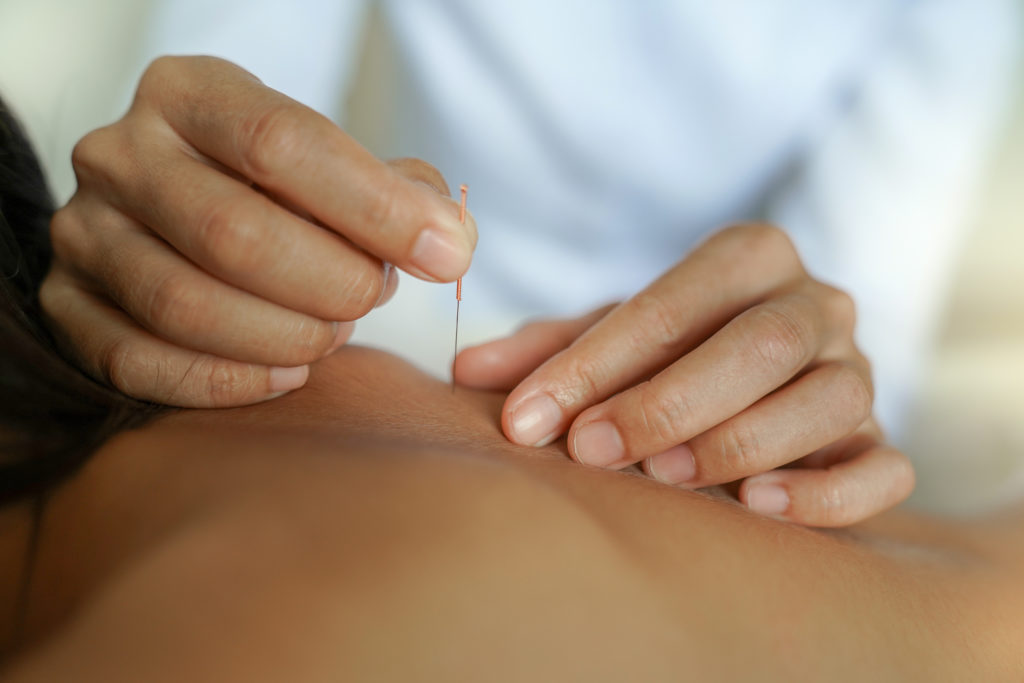
Current dry needling done by physiotherapists uses about 6 short needles per session, only addressing a negligible fraction of all the trigger points that may be contributing to your pain condition. My mother uses 60-70 needles of different lengths per session, slowly introducing the needles and leaving them in for about 30 mins, as opposed to quickly pumping them in and out, as is done in the US – it’s a completely different technique in her hands.
These past few years, we have been working towards finding a pathway to train qualified US-based professionals to do USGDN. It requires both requires ultrasound training and an extremely thorough re-grounding in muscle anatomy for physicians and an even more extensive training for non-physicians.
It has been a long, uphill arduous path with little success until now. It is also hampered by the fact that there is no incentive for medical professionals here to do a low-cost intervention such as dry needling – the medical economics don’t make sense. What is picking up is botox injection for trigger points, because it is a technique that can be billed at a much higher rate than dry needling.
If anyone is looking for DN as described above as a treatment for their chronic pain, I would consult this pain physician in Dallas. He also practices regenerative medicine, which may marry very well with USGDN (which itself promotes muscle healing) to produce even more spectacular results.
As a note, USGDN or other treatments (such as botulinum toxin injection) that relieve trigger points can help with cancer pain (see here and here), which has now shown to be partly myofascial in origin, complex regional pain syndrome, interstitial cystitis, migraines, trigeminal neuralgia, piriformis syndrome (a type of sciatica), lower back or disc pain, abdominal and visceral pains, knee pains (both osteoarthritis and rheumatoid arthritis), writer’s cramp, carpal tunnel, and so many other conditions.
Myofascial pain solutions to try at home
This post is not just about unicorns you can’t catch quite yet. USGDN as done in the comprehensive protocol discussed above will not be an option available to most patients, though dry needling with about 6 needles per session by physiotherapists is available, and may help to a small degree. Sitting at home, what can you do to partially relieve your pain? I live far away from my mother and suffer from back and neck pain (I develop trigger points just by merely existing, maybe also due to food allergies), and all of these approaches in combination help me chip away at the iceberg if it ever gets too big:
TENS (transcutaneous electrical nerve stimulation): TENS for pain is commonly used by physiotherapists. It produces electrical impulses through electrodes placed on the surface of your skin. The electrodes are placed at or near nerves where the pain is located or at trigger points. I’m not quite sure how it does it, since it stimulates sensory nerves, but TENS seems to relax my muscles, and has helped a lot of people worldwide ease their pain temporarily. TENS units are cheap, and largely safe except under certain conditions. Talk to your doctor or physiotherapist before you purchase!
Topical pain relievers for muscle pain: I have found a mixture of Penetrex, magnesium oil, and turmeric essential oil to really reduce local inflammation and pain – more in this post!
Oral Magnesium Supplements: Magnesium deficiency is widespread, and supplementation may improve muscle tightness and improve sleep, which is often impacted when you have muscle pain, which creates is a vicious cycle in itself. This is my tried-and-tested Magnesium supplement – multiple family members have told me they have felt perceptibly better after taking this one.
Fixing Deficiencies: Vitamin D and Vitamin B-12 deficiencies are common, and very strongly related to chronic pain syndromes. My mother finds that literally every one of her chronic pain patients is Vitamin D and Vitamin B-12 deficient. Fixing the deficiency cannot cure the pain syndrome in itself, but is likely necessary to prevent pain recurrence.
Turmeric for rheumatoid arthritis/osteoarthritis pains: In addition to the topically applied triple combination of Penetrex, magnesium oil, and turmeric essential oil, orally consuming turmeric, which is potently anti-inflammatory might help – mounting evidence suggests it reduces symptoms in rheumatoid arthritis and osteoarthritis. Turmeric however has bad bioavailability, and you need to take a formulation that will be well absorbed and well-retained. I like these two oral supplements: liposomal curcumin and turmeric in coconut oil with black pepper.
Hope some of this helps! I love hearing anecdotal reports of how these suggestions help, so if you try any of the at-home ideas provided above, please come back and let me know how it worked out!















